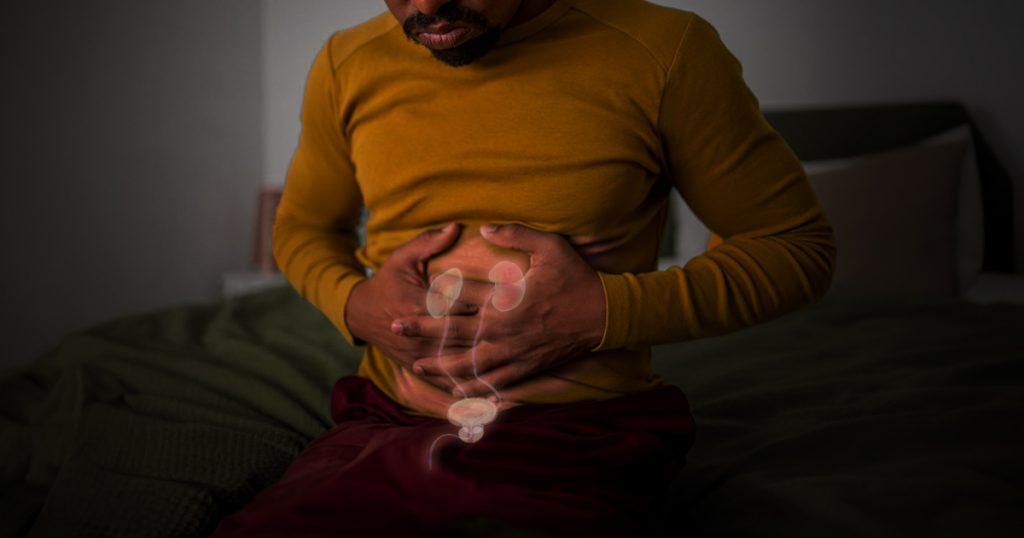
Prostatitis is a prevalent condition that affects the prostate gland, a small walnut-shaped organ situated below the bladder in men. As an essential part of the male reproductive system, the prostate gland produces seminal fluid, which nourishes and transports sperm. When inflammation occurs within this gland, it can lead to various symptoms that impact different aspects of a man’s life.
These symptoms may include pain in the pelvic region, lower back, or genitals, difficulty urinating, frequent urination, especially at night, and sexual dysfunction, such as painful ejaculation or erectile dysfunction. By intervening early in the course of prostatitis, patients can experience relief from these symptoms, prevent further complications, and improve their overall quality of life.
Exploring the Different Types of Prostatitis
Prostatitis is not a one-size-fits-all condition. This condition can be categorized into four unique types, each possessing its own set of features, causes, and treatment strategies. Understanding these different types of prostatitis can help healthcare providers tailor their diagnostic and therapeutic strategies to best address the specific needs of each patient.
1. Acute Bacterial Prostatitis
Acute bacterial prostatitis results from a sudden bacterial infection in the prostate gland. Although this type is the least common, it can be severe and necessitates prompt medical attention. Symptoms include high fever, chills, painful urination, and pelvic or lower back pain. The usual treatment for this condition includes antibiotics to address the root cause of the infection, as well as pain management and supportive care.
2. Chronic Bacterial Prostatitis
Chronic bacterial prostatitis is characterized by recurrent bacterial infections in the prostate gland. While it shares some similarities with acute bacterial prostatitis, the symptoms are usually milder and develop more gradually.
Individuals suffering from this condition might encounter recurrent urinary tract infections, painful urination, and discomfort in the pelvic area. Long-term antibiotic therapy is often prescribed to treat this type of prostatitis, though it may be challenging to eradicate the infection completely.
3. Chronic Pelvic Pain Syndrome (CPPS)
The most prevalent form of prostatitis is chronic pelvic pain syndrome, also referred to as chronic nonbacterial prostatitis. As the name suggests, it is not associated with a bacterial infection. The exact cause of CPPS remains unclear, but it may be related to factors such as muscle tension, nerve dysfunction, or inflammation.
Individuals with CPPS frequently suffer from persistent pelvic pain, urinary issues, and sexual dysfunction. To manage symptoms and enhance the quality of life, treatment for this type of prostatitis may comprise a mix of medications, physical therapy, and lifestyle changes.
4. Asymptomatic Inflammatory Prostatitis
Asymptomatic inflammatory prostatitis is a unique type in which patients have inflammation in their prostate gland but do not experience any symptoms. This type of prostatitis is often discovered incidentally during routine examinations or while investigating other medical issues. Since it does not cause any noticeable discomfort or complications, asymptomatic inflammatory prostatitis typically does not require treatment.
Significance of PSA Testing in Prostatitis Diagnosis
Prostate-specific antigen (PSA) is a protein produced by the prostate gland. When there is inflammation or infection in the prostate, as seen in prostatitis, PSA levels in the blood can rise. Therefore, an elevated PSA level may indicate the presence of prostatitis, warranting further investigation.
It is important to note that while PSA testing can be a valuable tool in identifying potential cases of prostatitis, it should not be relied upon as the sole diagnostic method. Rapid rise in PSA levels may also be attributed to other conditions like benign prostatic hyperplasia (BPH) or prostate cancer. To correctly diagnose prostatitis, a thorough assessment is vital, encompassing a comprehensive medical history, physical examination, and supplementary tests.
Interpreting PSA Levels: How High Can PSA Levels Go With Prostatitis?
There is no definitive PSA level threshold that confirms prostatitis. PSA levels can significantly vary among individuals due to factors like age, ethnicity, and overall health. Generally, a PSA level above 4.0 ng/mL suggests an underlying prostate problem and warrants further testing. However, it’s important to note that a level below 4.0 ng/mL doesn’t eliminate the possibility of having prostatitis.
Instead of focusing solely on a specific PSA level, healthcare providers should consider the patient’s overall clinical picture when evaluating the likelihood of prostatitis. This approach may include assessing the rate of change in PSA levels over time (PSA velocity), as rapidly increasing levels may be more suggestive of prostatitis or other conditions requiring further investigation.
Proper Diagnosis of Prostatitis
A thorough and comprehensive approach is necessary for accurately diagnosing prostatitis. The process typically involves the following steps:
1. Medical history and symptom assessment
Initially, the healthcare provider will inquire about the patient’s symptoms, medical background, and any potential risk factors associated with prostatitis. This information helps determine the likelihood of prostatitis and guides further diagnostic procedures.
2. Physical examination
A digital rectal exam (DRE) is often performed to assess the prostate gland. In this examination, the healthcare provider introduces a gloved, lubricated finger into the rectum to detect any abnormalities, like swelling or tenderness, within the prostate.
3. Laboratory tests
The healthcare provider may order urinalysis and urine culture to look for indications of infection or inflammation. Blood tests, such as PSA testing, can also offer valuable insights into the patient’s overall health and assist in ruling out other conditions.
4. Imaging studies
In some cases, imaging studies such as ultrasound or magnetic resonance imaging (MRI) may be necessary to visualize the prostate gland and surrounding structures, providing further insight into the underlying cause of the patient’s symptoms.
5. Additional tests
Depending on the findings from the initial evaluation, additional tests may be recommended to confirm the diagnosis or rule out other conditions. These tests may include semen analysis, post-prostatic massage urine test, or cystoscopy.
Effective Treatment Strategies for Prostatitis
Once a diagnosis of prostatitis has been established, the healthcare provider will develop a personalized treatment plan tailored to the specific type and severity of the condition. Treatment options may include:
1. Antibiotics
For bacterial prostatitis (acute or chronic), antibiotics are prescribed to target the underlying infection. The duration of antibiotic therapy can range from a few weeks to several months, depending on the severity and type of infection.
2. Anti-inflammatory medications
Non-steroidal anti-inflammatory drugs (NSAIDs) may be beneficial in relieving pain and inflammation related to prostatitis.
3. Alpha-blockers
These medications can help relax the muscles around the bladder and prostate, improving urinary symptoms associated with prostatitis.
4. Pain relievers
Over-the-counter pain medications or prescription analgesics may be recommended to manage pain and discomfort.
5. Physical therapy
Pelvic floor exercises and other forms of physical therapy can help alleviate muscle tension and pain associated with chronic pelvic pain syndrome (CPPS).
6. Lifestyle modifications
Patients may be advised to make certain lifestyle changes, such as avoiding caffeine, alcohol, and spicy foods, which can exacerbate prostatitis symptoms. Regular exercise, stress management, and proper hydration can also contribute to symptom improvement.
Understanding the Connection Between a Sudden Rise in PSA & Prostatitis
In summary, it is essential to recognize the potential link between a sudden rise in PSA levels and prostatitis. While elevated PSA levels can be indicative of various conditions, such as benign prostatic hyperplasia (BPH) or prostate cancer, a rapid increase in PSA may be more suggestive of prostatitis. When assessing patients exhibiting urinary symptoms or pelvic pain, healthcare providers should take this information into account.
It is crucial to remember that PSA testing alone cannot provide a definitive diagnosis of prostatitis. To accurately diagnose and treat this condition, a comprehensive approach is essential, encompassing a detailed medical history, physical examination, and supplementary tests. By understanding the connection between a sudden rise in PSA levels and prostatitis, healthcare providers can better identify and manage cases of prostatitis, ultimately improving the quality of life for men affected by this condition.